News and blogs
241 articles
 News
NewsFormal ministerial approval for merger by acquisition
Announcement of merger by acquisition of the Tavistock and Portman NHS Foundation Trust
 News
NewsWatch Me Play! Learning from research
An important research paper on Watch Me Play! has just been published in the Journal of Child Psychotherapy.
 News
NewsSocial work conference: From performance culture to “good enough” practice
Social work conference explores what helps social workers stay relational
 News
NewsSupporting young people with eating difficulties
Across the UK, growing numbers of children are experiencing eating disorders, with demand for specialist services rising sharply since the pandemic.
 News
NewsPerinatal mental health training key as Family Hubs expand
Perinatal mental health experts are urging services to prioritise specialist training for their workforce...
 News
NewsTavistock and Portman to merge with North London NHS FT
The Tavistock and Portman is one step closer to merger with NLFT following approval from both boards and councils of governors.
 News
NewsNew research highlights role of shame in treating antisocial personality disorder
A new study published in the Journal of Clinical Psychology, January 2026, edition offers fresh insights into the treatment of antisocial personality disorder
 News
NewsFrom shell shock to the science of attachment: The Tavistock and Portman’s century of talking therapies
Time to Talk Day (5 February 2026) is the biggest mental health conversation of the year, and we’re reflecting on over a century of talking therapies.
 News
NewsEmpowering parents through the incredible years parenting group
Our Mental Health Support team have been running the Incredible Years parenting group, a programme designed to support parents and carers.
 News
News2025 publishing successes
Publishing and research have flourished at the Tavistock and Portman in 2025. Here are some of the highlights.
 News
NewsA breakthrough for treating antisocial personality disorder
Groundbreaking research by the Portman Clinic and UCL published in The Lancet offers evidence that MBT adapted specifically for ASPD can make a real difference
 News
NewsTavistock trauma specialists welcome new strategy to tackle violence against women and girls
Experts from the Tavistock and Portman NHS Foundation Trust have welcomed the government’s new violence against women and girls (VAWG) strategy.
 News
NewsArt exhibition: John Roper, “And the Coronation will be Televised”
A photography exhibition by John Roper is on display at the Tavistock Centre during January 2026.
 News
News90 Years of research at the Tavistock and Portman
This year marks 90 years since the Tavistock and Portman began formal research – a tradition that continues to shape mental health care worldwide.
 News
NewsInternational trauma conference: a global exchange of ideas
The Tavistock Trauma Service in collaboration with the South Africa Psychoanalytic Clinics hosted the first International Psychoanalytic Trauma Conference.
 News
NewsArt exhibition: Marcus Price “Captivity and Freedom”
Art exhibition: Marcus Price “Captivity and Freedom”
 Blog
BlogReflections from our Lead Governor Kathy Elliott for 2024/25
Our Lead Governor Kathy Elliott, recently spoke at our Annual Members’ Meeting and reflected on her highlights for 2024/25.
 News
NewsCelebrating recent staff and alumnus book releases
Books showcasing how psychotherapy continues to shape both clinical practice and leadership development have recently been published.
 News
NewsAruna Mehta appointed as interim Chair
Aruna Mehta has become interim chair of the Tavistock and Portman NHS Foundation Trust.
 News
NewsAnnual members’ meeting 2024/25
Our annual members' meeting took place on Thursday 30 October where we looked back at our performance and achievements of 2024/25.
 News
NewsArt exhibition: Corridor Garden by Jolene Liam
Jolene Liam, a Singaporean artist and architect, is exhibiting her drawing series ‘Corridor Garden’ at the Tavistock Centre.
 News
NewsChildren of parents with a mental illness recognised in new statutory guidance
The UK Government has agreed to a landmark amendment to the Mental Health Bill 2025, recognising children of parents with a mental illness.
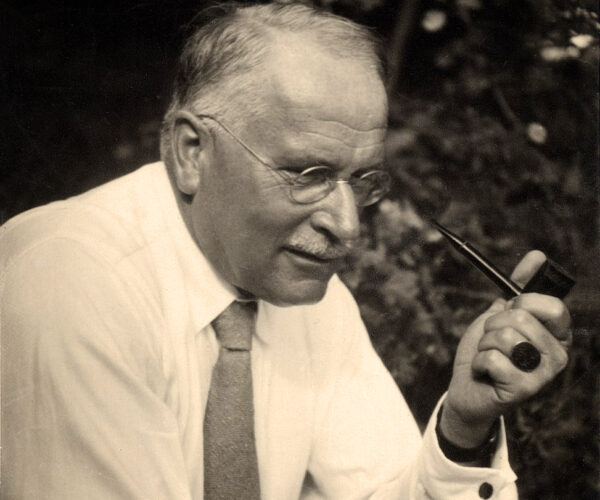 News
NewsNinety years on: Jung at the Tavistock
This year marks the 90th anniversary of Swiss psychiatrist and psychoanalyst Carl Jung’s famous series of lectures at the Tavistock Clinic in London
 News
NewsBefore people see the autism, they see my race
Exploring the lived experiences of Black autistic girls, addressing a significant gap in autism research, educational and psychological practice.
